A new study by scientists at the University of Edinburgh and published on the preprint server medRxiv* in July 2020 suggests an interesting link between ultraviolet A radiation and deaths due to COVID-19. While this is an observational study, which means that direct inferences cannot be drawn from this finding, it does, however, suggest better strategies for reducing the death rate due to COVID-19.

Study: Ultraviolet A Radiation and COVID-19 Deaths: A Multi-Country Study. Soloviova Liudmyla / Shutterstock
The COVID-19 pandemic is still spreading throughout many countries, and scientists are exploring its risk factors as part of the effort to contain the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). Among the variables being considered are seasonal variations, temperature and humidity conditions, and ultraviolet irradiation. These are known to play a role in several infectious diseases already, such as influenza.
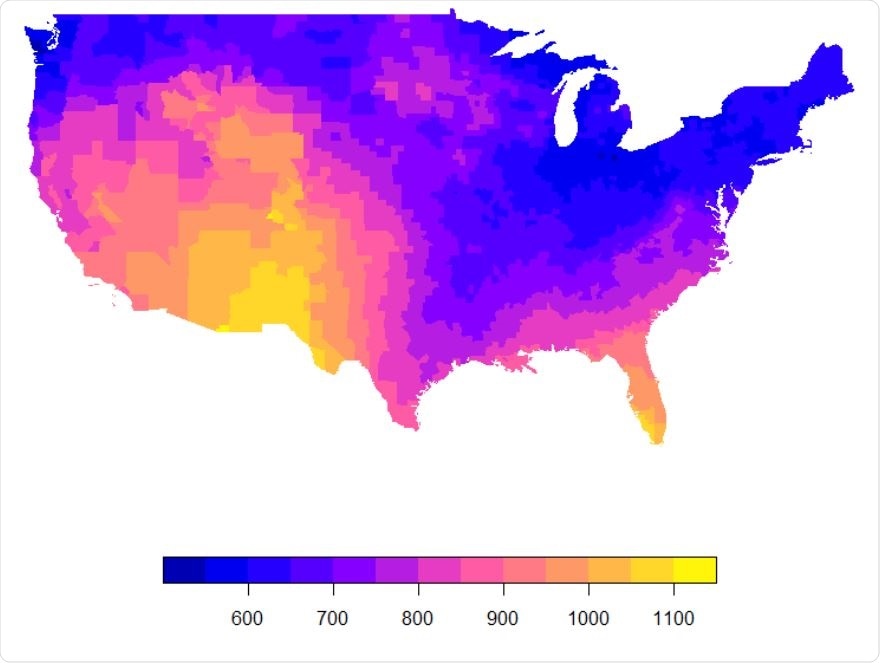
Daily mean UVA (KJ/m2 ) in the contagious USA between Jan-Apr 30th 2020.
Ultraviolet, Sunlight and COVID-19
Since the current pandemic has not yet completed one cycle of seasons, all these factors cannot be thoroughly evaluated. However, the level of ultraviolet (UV) irradiation in the atmosphere can be studied in relation to COVID-19 death rates.
Previous research by the same team showed that sunlight can reduce blood pressure via nitric acid production, independent of vitamin D levels. Population-wide studies show that increased UV levels are related to lower blood pressure and decreased heart attack rates. This could also cause diabetes and metabolic syndrome incidence rates to fall.
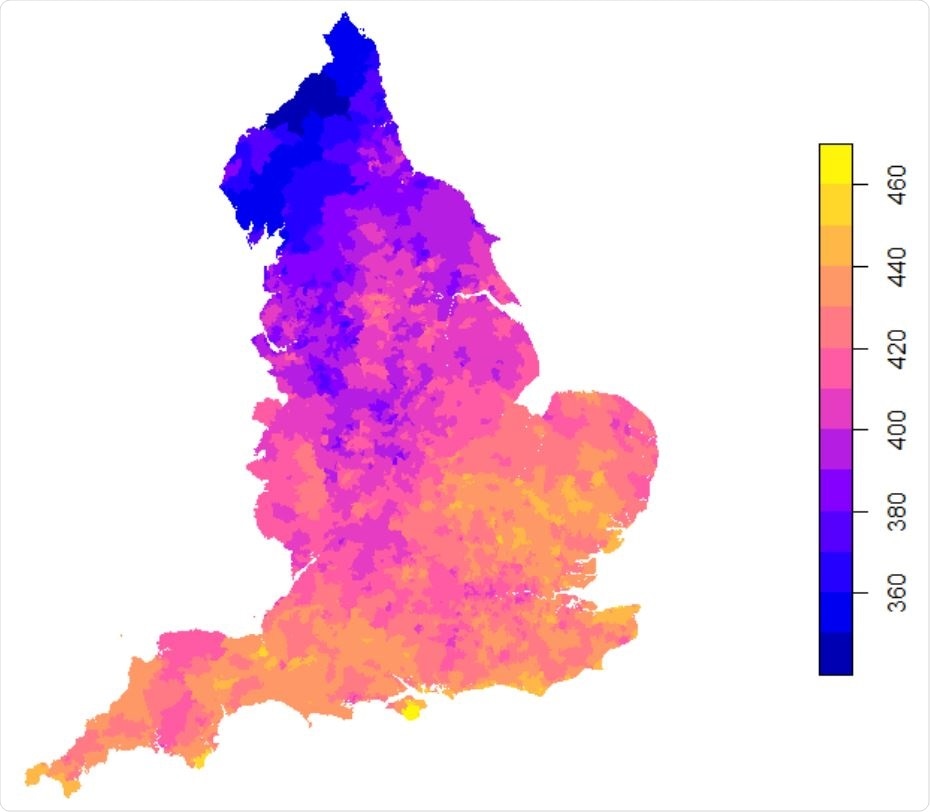
Daily mean UVA (KJ/m2 ) in England between Jan 1st -Apr 17th 2020
The Study: UV and COVID-19 in 3 Countries
Since COVID-19 disease appears to have greater severity among people with these conditions, the current study explores the association between ambient UV and COVID-19 deaths in three countries, namely, the USA, England, and Italy. It looks at over 11,000 counties and areas in these countries in three independent data sets, using only those counties where the UV level was below the threshold known to induce significant vitamin D3 biosynthesis in the skin.
This threshold corresponds to a monthly mean vitamin D effective UV (UVvitd) of under 165 KJ/m2. This period is termed the UV vitamin D winter and covered the months from January to April 30, 2020. The daily UV irradiance was derived from satellite data, after accounting for atmospheric absorption by water vapor and ozone.
The researchers found that the daily mean UVA levels hovered between 450 to 1,000 KJ/m2 across these countries.
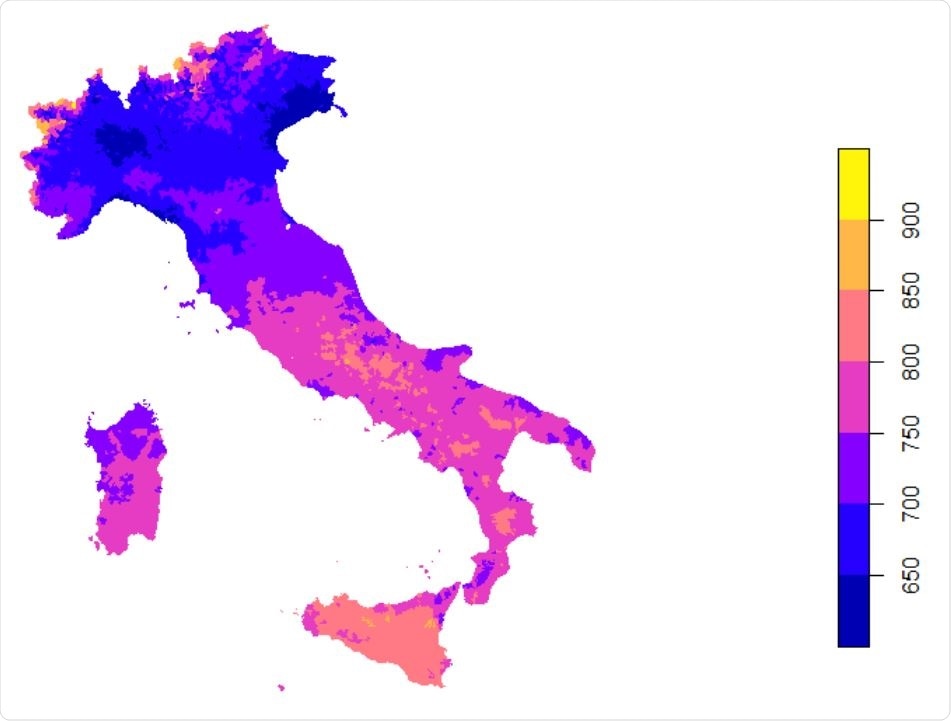
Daily mean UVA (KJ/m2 ) in the Italy between Jan 1st - Apr 30th 2020
After adjusting for demographic, socioeconomic, susceptibility, and long-term environmental variables, the researchers arrived at a multivariate analysis outcome. These include the percentage of older people, ethnic composition, low income and poverty indicators, air pollution indicators such as PM2.5, which reflects fine particulate matter in the air, and the susceptibility to infection. The latter was calculated from various factors such as the population density coupled with the percentage of positive tests and exposure in various ways, as by public transport.
UVA Reduces COVID-19 Mortality
The model shows that UVA levels are inversely related to COVID-19 mortality. The mortality risk ratio (MRR) is 0.73, which reflects a 27% reduction in risk with an increase of 100KJ/m2 in UVA irradiation in the USA. In England and Italy, it is 0.51 and 0.81 respectively, which means a reduction in deaths by 49% and 19% respectively. Overall, therefore, the MRR was 0.68.
This effect is independent of both cold temperatures and of whether the UVA ambient levels crossed the threshold for vitamin D synthesis. An interesting finding is that the higher UVA levels produced more significant reductions in mortality risk in countries with a lower average UVA level, namely, England, compared to the USA or Italy, which have higher average ambient UVA.
Mechanisms of Action
The researchers suggest that UVA may act via several mechanisms. For one, the irradiation may inactivate the virus in airborne droplets and fomites, reducing the rates of spread and the size of the inoculating dose in those coming into contact with infectious material. This would lead to less severe infection.
Secondly, UVA induces the release of nitric oxide from the skin, which then enters the bloodstream, causing blood vessels to dilate and reducing the blood pressure. This, in turn, promotes cardiovascular and metabolic health. This produces a reduction in the risk of death from COVID-19 since heart disease, vascular conditions, and metabolic syndrome are high-risk factors.
Thirdly, UVA may reduce the replication of the virus. In SARS-CoV, it acts by s-nitrosating the spike protein, which means it cannot bind with its receptor, the angiotensin-converting enzyme (ACE) 2. Both SARS-CoV and SARS-CoV-2 have homologous spike proteins, and hence this action could be present in the latter as well.
Fourthly, endothelial damage, and impaired endothelial nitric oxide synthase activity could be the underlying reason for extensive organ damage in severe COVID-19. UVA could reduce this as well, by promoting the photochemical reaction that produces more nitric oxide.
Future Research and Conclusion
The study concludes, “Our analysis, replicated in 3 independent national datasets, suggests ambient UVA exposure is associated with lower COVID-19 specific mortality.”
The next step would be to confirm that this is a causal association. If so, this could be an easy way to reduce the mortality from the pandemic by advising optimal sun exposure. Moreover, the independent mechanisms could be replicated therapeutically, especially those involving circulating nitric oxide.
*Important Notice
medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.