Researchers at the National Institute for Public Health and the Environment in the Netherlands say that airborne transmission of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) is possible and should not be discounted.
The team’s data showed that sneezing is associated with the most significant probability of aerosol exposure, followed by coughing, speaking, and breathing.
A pre-print version of the paper is available on the server medRxiv*, while the article undergoes peer review.
.jpg)
Speculation about airborne transmission
Ever since the coronavirus disease 2019 (COVID-19) outbreak began in Wuhan, China, late last year, scientists have been debating the extent to which SARS-CoV-2 can be transmitted via aerosols (particles suspended in the air).
The World Health Organization still maintains that the virus is not airborne. Still, researchers warn that airborne transmission should be considered as a potential explanation for why COVID-19 has spread so quickly.
If SARS-CoV-2 is spread in this way, this would have implications regarding the measures that are currently taken to limit transmission. For example, “transmission would be plausible beyond the often advised 1.5 meters,” say Schijven and team.
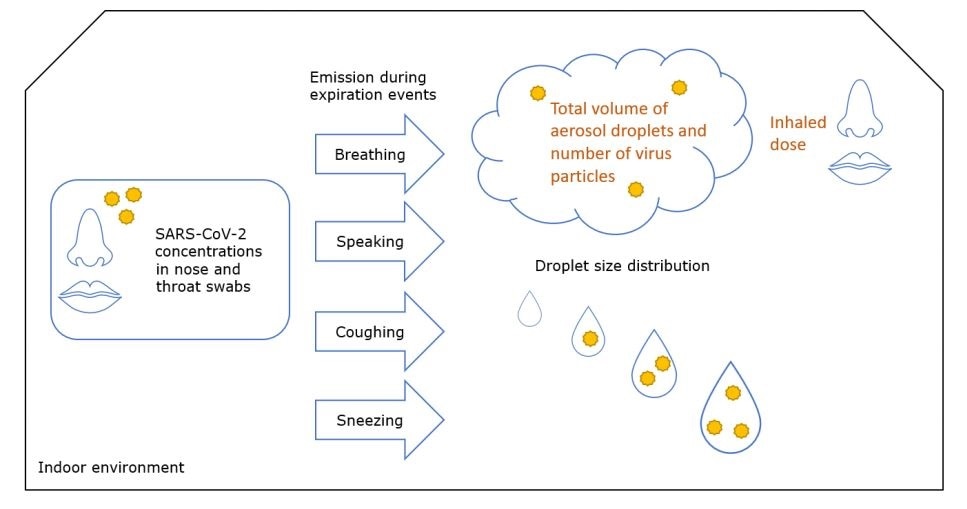
Overview of the processes modeled in this study.
The current recommendations
People are currently advised to stay at home if they are sneezing or coughing, but it is also known that high viral loads can occur before or during the very first days of symptom onset.
“Therefore, an occasional sneeze or cough could easily occur before one realizes one should have stayed at home,” say the authors.
Given that coughing is a primary symptom of COVID-19 and that a person may cough many times in a row, it could be assumed that coughing may be more of a concern than sneezing, notes the team.
Furthermore, singing, speaking loudly, and even heavy breathing can all expel virus particles into the air.
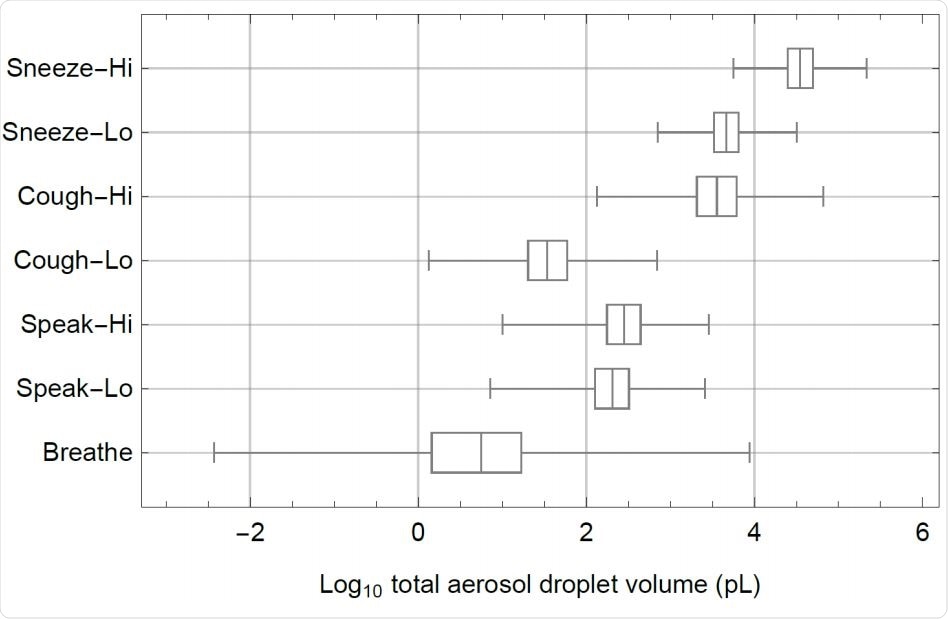
Box-whisker chart of the log10 of total aerosol droplet volumes (pL=picolitres) that are expelled in each scenario (Table 1), showing median values, quartiles (boxes) en minimum and maximum values (whiskers). Volumes in pL/20 minutes for breathing and speaking and in pL per cough and per sneeze.
Factoring in droplet size
The fate of infected droplets expelled into the air depends on their size. Larger droplets my fall to the ground more quickly than smaller ones that may stay suspended as aerosols for more extended periods.
It is known that airborne particles can penetrate the lungs more deeply, while bigger particles are more likely to affect the upper airways. However, “while it is true that the large majority of the volume of fluids that are expelled during, for example, coughing and sneezing, is in droplets that deposit quickly, this does not imply that airborne transmission is highly unlikely,” writes the team.
What did the study involve?
Schijven and colleagues developed an exposure assessment model that enabled them to estimate how many SARS-CoV-2 particles are present in airborne particles expelled as a result of breathing, speaking, coughing, and sneezing.
The assessment involved estimating the number of particles expelled by an infected person in an unventilated, indoor setting, and subsequent inhalation by at least one other person in the same environment. Various scenarios were incorporated, including different room sizes, exposure times, and viral concentrations.
What did the study find?
The team found that sneezing expelled the greatest volume of aerosol droplets. This was followed by coughing, speaking for 20 minutes, and breathing for 20 minutes.
The number of particles expelled ranged from a few million to as much as a hundred million.
The researchers say the findings suggest that the number of viral RNA copies in one milliliter of mucus can be as high as 10 million in one-fifth of cases and as high as 100 million in five percent of cases. This can probably even be the case when people are asymptomatic, which increases the likelihood of exposure, they add.
The probability of exposure varied depending on the concentration of SARS-CoV-2 in mucus and the scenario. Still, overall, the probability was generally less than 1% if the concentration was less than 100,000 per mL.
“It is recommended to be precautious”
However, the team points out that it is not known exactly what fraction of airborne RNA-copies are infectious and that observational studies on infectious viruses in aerosols are needed to validate modeling efforts.
“Aerosol transmission of SARS-CoV-2 is possible and should not be disregarded,” write Schijven and colleagues.
So long as it is uncertain what fraction of the airborne virus particles is infectious, “it is recommended to be precautious,” concludes the team.
*Important Notice
medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, should not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.